Even though short-term use of unopposed estrogen therapy does not appear to increase the risk of breast cancer, the impact of longer-term estrogen therapy use is somewhat unclear. This study investigates the possible link between the longer-term use of unopposed estrogen therapy and the risk of invasive breast cancer over an extended follow-up period. It takes into account other possible contributing factors such as age at menopause and whether or not this increases the risk of invasive breast cancer. This investigation evaluates the association of longer-term estrogen therapy and breast cancer in a large group of women, all of whom have been through menopause.
In 1990, breast cancer risk factors among female participants in this study, all of whom had been through menopause, varied in terms of use and duration of estrogen therapy. In a number of categories, such as age and age at menopause, women who had never tried estrogen therapy were similar to women who had used estrogen therapy for over 10 years, but varied from those who currently used estrogen therapy for less than 10 years.
It was found that women who had gone through menopause and never tried estrogen therapy were less likely to have history of benign breast disease or to have undergone screening within the previous 2 years, and more likely to have a family history of breast cancer. Females who had gone through menopause and who had used estrogen therapy for more than 10 years were slimmer and more likely to have had a bilateral salphingo-oophorectomy, which is generally thought to reduce the risk of breast cancer.
Predictably, for women who had gone through menopause and had used estrogen therapy for 20 years or longer, the correlation seemed stronger for estrogen receptor (ER) or progesterone receptor (PR) cancers.
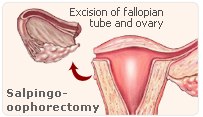
Current estrogen therapy users at this time were also more likely to have had a bilateral salpingo-oophorectomy and to have started menopause at an earlier age, and therefore may have lowered their risk of breast cancer compared with women who had undergone menopause but never used estrogen therapy.
Among women who used estrogen therapy for less than 20 years, no significant increased risk of breast cancer was observed overall. Though, there was a greater risk with longer durations of use, primarily for ER+/PR+ cancers.
This study shows that there is indeed a link between length of estrogen therapy use and increased risk of invasive breast cancer. This data indicates that longer-term use increases the risk of invasive breast cancer. This association appeared more prominent in slender women and for ER+/PR+ cancers. Despite the fact that existing use of estrogen therapy for less than 10 years was not linked with a statistically momentous increase in breast cancer risk, the WHI demonstrated an increased possibility of stroke and deep-vein thrombosis in the same time frame. Thus, females using estrogen therapy to prevent or treat osteoporosis typically need longer-term treatment, and are therefore recommended to investigate other options, given the increased risk of breast cancer with longer-term use of estrogen therapy.