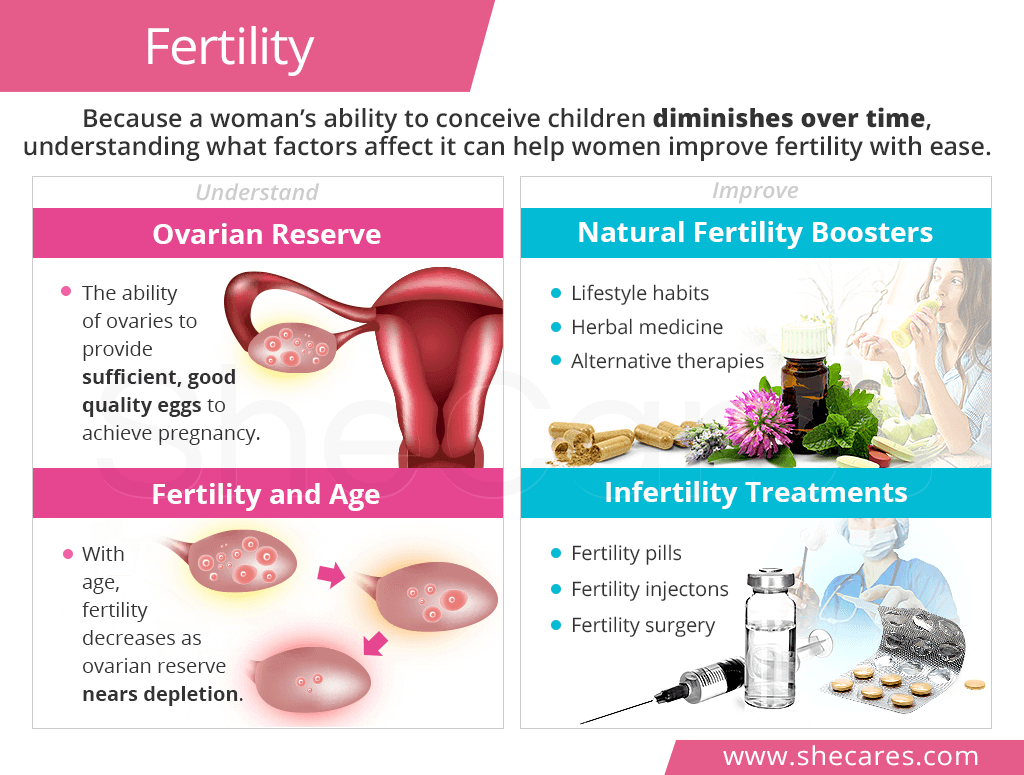
Ovarian Reserve: Female Egg Count and Quality
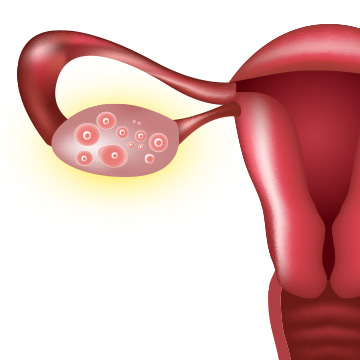
Fertility in women mainly depends upon their ovarian reserve.
Ovarian reserve is the ability of the ovaries to provide a sufficient number of good eggs that can develop into a healthy pregnancy.
It has two key components, egg quantity and egg quality, both of which undergo a gradual decline over time:
Egg Quantity
Also called egg count, it is the number of eggs in the ovaries, which serves as a woman's lifetime supply.
Egg quantity decreases at various rates throughout a woman's life stages. During fetal development, the ovaries contain up to six million eggs. With time, the ovarian reserve moves towards total depletion at menopause.
Egg Quality
The term egg quality refers to the chromosomal make-up of the eggs, which determines whether they can lead to a healthy pregnancy.
Ovarian eggs age similarly to other cells in the body. Over time, there are natural changes in the DNA composition of the eggs due to illnesses, fever, toxin exposure, etc. An abnormal egg released on ovulation might fail to be fertilized or implanted in the uterine wall. It can also lead to pregnancy complications, such as miscarriage or birth defects.
Low Ovarian Reserve
A low ovarian reserve occurs when there is not enough good quality eggs in the ovaries to achieve pregnancy.
This decline in the quality and quantity of ovarian eggs is a natural process occurring at various rates from woman to woman. Generally, after the age of 35 or 10-15 years before menopause, fertility starts to decline faster.
Click on the following link to read more about ovarian reserve or proceed to the next section to read about the relationship between fertility and age.
Fertility and Age
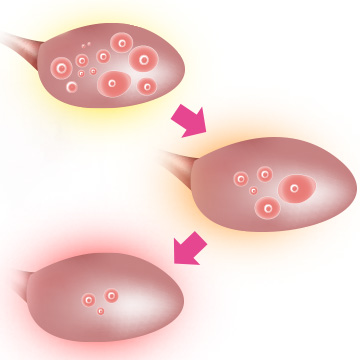
Age is the most important factor affecting female fertility, and a natural decline in the ability to conceive occurs at different rates at various ages.
Fertility Rates in the 20s
Women in their 20s have the highest fertility rates.
Ovarian reserve is in great shape, which means that eggs are abundant, and the majority do not have chromosomal abnormalities. As a result, 25% of women in their 20s conceive in any given cycle, and normally all do so within a year.
Fertility Rates in the 30s
Turning 30 is usually the first time women start wondering about their fertility.
Generally, women in their 30s have high chances of conceiving and having healthy pregnancies, especially in early 30s. However, fertility at 35 brings new reproductive challenges as ovarian reserve begins to decline at faster rates. As a result, miscarriage and birth defect risks increase in mid-30s.
Fertility Rates in the 40s
Getting and staying pregnant after 40 is much more difficult as the egg count decreases rapidly, and the majority of eggs have chromosomal abnormalities.
Although fertility at 40 can still lead to a healthy pregnancy, conceiving naturally after 45 is almost impossible. This is because women typically enter the menopausal transition at this age, during which hormonal fluctuations cause irregular periods and ovulation problems.
As a result, women in their 40s rely heavily on the use of assisted reproductive technologies (ARTs).
Fertility Preservation
Because age-related fertility decline is inevitable, women might choose to prolong their fertility and postpone getting pregnant for later through fertility preservation methods.
Fertility preservation is the process in which eggs or reproductive tissues are saved for future use.
Egg Freezing
There are two ways in which a woman's eggs can be frozen. The most common one, called embryo cryopreservation, consists of extracting the eggs from the ovaries, fertilizing them through IVF, and then freezing them. When a woman is ready for pregnancy, the fertilized eggs are placed in the uterus for implantation through IVF.
The second egg freezing technique is called oocyte cryopreservation. It involves the same steps with the exception that the eggs are stored unfertilized. With this method, before the eggs are placed in the uterus, they have to be fertilized in the lab.
Gonadal Shielding
It is designated for women undergoing radiation treatment. Because the rays can cause damage to the reproductive organs, the pelvic area is protected with a lead shield. The specific shielding technique used by fertility specialists is an important factor determining the effectiveness of this fertility preservation method.
Ovarian Transposition
It consists of surgically moving the ovaries and the fallopian tubes away from the area where radiation will be directed. This option is often used for young cancer patients to preserve their fertility.
Some women decide to undergo fertility preservation because they do not feel ready for pregnancy due to various life situations, like careers, relationships, or finances, while others might be going through cancer treatment known to have detrimental effects on female fertility.
Fertility Tests
At-home and medical fertility tests are used to assess fertility in women.
Home Fertility Tests
At-home fertility tests detect ovulation signs and symptoms to determine when a woman is ovulating in order to time having intercourse with her fertile window more precisely.
Over-the-Counter Fertility Tests
The most common store-bought fertility tests are ovulation test kits, which detect the LH surge (luteinizing hormone) in urine right before ovulation. Others, such as ovulation microscopes, work by detecting ferning patterns in saliva due to rising estrogen leading up to the egg release.
Self-Assessment Fertility Tests
Observing body hints about ovulatory patterns includes measuring basal body temperature, the rise of which is caused by rising progesterone upon ovulation. Checking cervical mucus or cervix position during cycle can also give clues about a woman's fertility and help detect ovulation problems.
Medical Fertility Tests
Women who did not get pregnant after a year of trying are advised to undergo medical fertility tests to pinpoint the exact cause of infertility.
Pap Smear
This standard gynecological exam is used to rule out cervical problems as well as sexually transmitted diseases (STDs) that might be lowering fertility.
Blood Tests
They are used to rule out hormonal imbalance as the cause of infertility. They most commonly measure the levels of anti-Müllerian hormone (AMH), day 3 FSH, and estradiol, which can give clues about the state of one's ovarian reserve.
Diagnostic Tests
Fertility testing always includes transvaginal ultrasounds to assess how many follicles are maturing in the ovaries and to rule out anatomical problems with the reproductive tract. Further investigations might include a hysterosalpingogram and hysteroscopy, among others.
Genetic Testing
DNA analysis is done on both parents when the aforementioned fertility tests failed to provide an explanation for lowered fertility. Genetic abnormalities account for 10% of infertility cases.
Infertility
Infertility is defined as the inability to conceive and carry on pregnancy. It is diagnosed when a woman has failed to get pregnant after 12 consecutive months of trying (or six months if older than 35).
Sterility, on the other hand, is diagnosed when conception does not occur because of lack of ovulation or sperm production due to genetics, disease, or injury.
Female Infertility
Female infertility is mainly caused by ovulation problems, which are rooted in hormonal imbalance manifested in various conditions, like polycystic ovary syndrome (PCOS). Fertility issues can also be due to fallopian tube blockage from endometriosis or an ectopic pregnancy. Factors such as advanced age or abnormal BMI can increase the risk of fertility problems.
Male Infertility
Issues with male fertility mainly concern sperm, including its production, delivery, or function. Most male infertility problems are caused by medical conditions or damage to the reproductive organs from radiation or injury. Obesity, alcohol use, or toxins can put men at higher risk of abnormalities.
Infertility Treatment
The choice of infertility treatment for women depends on the underlying cause, and it is designed to restore fertility.
Fertility pills and injections are the main treatments for ovulation induction.
Fertility surgery is aimed at restoring fertility by resolving structural abnormalities, like scarring or polyps.
Various natural ways, including diet, exercise, and alternative medicine, can also be effective in boosting fertility. They are discussed in the section below.
Boost Fertility

Because the female reproductive system runs on hormones, ensuring their balance can effectively boost fertility.
There are a variety of natural ways to increase fertility, including lifestyle habits, herbal medicine, and alternative therapies.
Lifestyle Habits
Through good daily practices, a woman can maintain proper nutrition and weight, both of which promote regular menstruation and healthy ovulation necessary for optimal female fertility.
Fertility diet consists of healthy fats (e.g. avocado, nuts), slow-release carbohydrates (e.g. whole grains, vegetables), and lean protein (e.g. beans, eggs). It should also include ovulation-friendly full-fat diary.
Fertility exercise increases blood flow to the uterus, encourages hormonal balance, and helps achieve a healthy weight. Moderate exercise, like swimming, should be chosen over extreme exercises to prevent ovulation disruption.
Herbal Medicine
There are numerous fertility vitamins and supplements that can resolve nutritional deficiencies behind fertility problems as well as act directly on the endocrine system to balance hormonal levels.
Hormone-balancing supplements, like Macafem, nourish the endocrine and pituitary glands to stimulate natural hormone production, increasing libido and boosting fertility.
Phytoestrogenic herbal supplements, such as dong quai or black cohosh, supply the body with plant-based estrogens to ultimately level out hormones, regulate ovulation, and support uterine function.
Fertility vitamins and minerals, like zinc, folic acid, or co-enzyme Q10, can increase the thickness of the uterine lining, improve ovulation egg quality, and reduce miscarriage risk.
Alternative Therapies
Promoting stress-free living can have positive effects on boosting fertility as prolonged stress can cause hormonal disruption and reduce a woman's state of being fertile.
Acupuncture can improve ovulation, increase blood flow to the uterus, and relieve the negative effects of cortisol levels on the female reproductive system, thus restoring fertility.
Mind-body techniques, such as meditation, mindfulness, and deep breathing exercises, have been shown effective for stress-reduction and restoring regular ovulation.
Conclusions
Many women take their fertility for granted until they decide to get pregnant and realize the complex mechanisms behind what it means to be fertile. This newly gained knowledge about the various factors affecting a woman's ability to conceive inspires many of them to make the most out of their pre-pregnancy planning and concentrate all efforts on preparing the mind and body for having a baby and giving him or her a head start in life.