Types of Ovulation Problems
There are two main ovulation problems women might experience:
Oligoovulation

Oligoovulation is characterized by irregular ovulation.
Egg maturation and release is taking place, but not on a regular, month-to-month basis. As a result, a woman might ovulate too early or too late in the cycle, or she might skip a month.
Irregular ovulation is common among pubertal girls and perimenopausal women due to natural hormonal fluctuations.
Anovulation
Anovulation is defined as lack of ovulation.
Sporadic anovulation happens occasionally throughout a woman's life and does not have any effect on her reproductive life. Chronic anovulation, on the other hand, occurs when there is no egg release for at least three consecutive months
Causes of Ovulation Problems
Ovulation problems are not a condition on their own. They are consequence of hormonal imbalance, which can be manifested in a variety of medical conditions, such as:
Polycystic Ovary Syndrome (PCOS)
PCOS is the most common cause of ovulation issues.
This endocrine disorder is characterized by abnormally high testosterone or insulin levels, irregular periods, and cysts in the ovaries. This consequently leads to an imbalance of other hormones, which might prevent the egg from developing and being released.
Hypothalamic or pituitary dysfunction
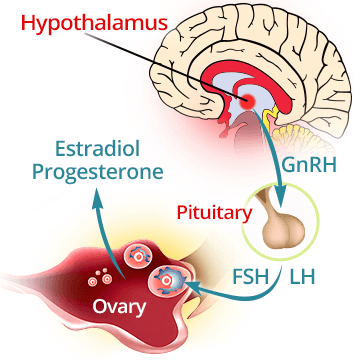
The release of key reproductive hormones needed for ovulation is governed by a synchronized and time-sensitive feedback mechanism, called the hypothalamic-pituitary-ovarian axis.
Any disruption along the pathway can affect the next step in the sequence of hormonal release, potentially delaying or preventing the maturation of the eggs or their release. Factors known to contribute to hypothalamic or pituitary dysfunction include abnormal body mass Index (BMI above 35 and below 18.5), high stress, or extreme exercise.
Endocrine disorders
Hyperprolactinaemia, high levels of prolactin hormone, might cause a decrease in reproductive hormones, leading to ovulation issues.
Thyroid dysfunction can lead to over- or underproduction of thyroid hormones, which leads to a malfunction of other key hormone-producing glands and organs, thus interfering with egg release.
Congenital adrenal hyperplasia is a genetic disorder characterized by irregular periods, ovulation problems, and fertility problems due to an overproduction of androgens.
Reproductive disorders
Premature ovarian failure is when ovaries stop producing enough estrogen and releasing eggs regularly before a woman is 40 years old. As a result, she experiences erratic periods and irregular ovulation.
Low ovarian reserve means that the supply of eggs in the ovaries - which would normally be released on ovulation - diminishes, resulting in infrequent or irregular ovulatory cycles. It is a natural phase in a woman's reproductive life.
Signs and Symptoms of Ovulation Problems
Generally, abnormal ovulation is not associated with clear symptoms, except for menstrual abnormalities.
However, it is possible for women to have regular menstruation and have ovulation issues or even not ovulate at all.
Symptoms of Ovulation Problems
Menstrual Abnormalities
- Irregular periods
- Absent periods
- Cycles shorter than 21 days
- Cycles longer than 35 days
- Excess hair
- Fatigue
- Irritability
- Digestive issues
Signs of Ovulation Problems
Hormonal imbalance
- FSH, LH, estrogen, progesterone, testosterone
- Thyroid-stimulating hormone (TSH)
- Prolactin
Other Associated Signs
- Ovarian cysts
- Lack of ovarian follicles
- Hirsutism
- Thyroid nodules
Since ovulation problems are a symptom of other medical conditions, they might be accompanied by signs and symptoms specific to them. This includes ovarian cysts or hirsutism with PCOS; or fatigue, irritability or depression with thyroid disorders; and more.
Tests for Ovulation Problems
Home Ovulation Tests

Because ovulation problems do not typically produce obvious symptoms, a woman might not know she is experiencing them. Self-assessing for the signs and symptoms of ovulation with home ovulation tests can allow her to catch any abnormalities in two to three cycles:
Measuring basal body temperature. When ovulation occurs, a rise in progesterone causes a small temperature increase. An absence of that rise can indicate that ovulation did not take place.
Checking cervical mucus. In the days leading up to ovulation, vaginal fluid changes to resemble an egg-white consistency. Lack of those cervical mucus characteristics can mean that a woman is not ovulating.
Checking cervical position. The cervix moves up higher into the body and becomes soft and open when a woman is the most fertile right before and on her ovulation day. Not being able to detect those changes can signal ovulation issues.
Ovulation test kits. An estrogen rise after period bleeding eventually triggers the LH surge, which prompts the ovary to release an egg. A lack of that LH spike can signify hormonal imbalance that disrupts ovulation.
Ovulation microscopes. Rising estrogen also changes electrolyte concentration in the saliva, producing observable ferning patterns, a lack of which is a sign of abnormal ovulation.
Women are encouraged to keep track of their periods so that data can be used for diagnosing ovulation problems, especially irregular ovulation. This can be done with ovulation predictors, such as calendars, calculators, trackers, or monitors, which can not only store the input menstrual data, but also help a woman predict her next ovulation date.
Medical Tests
Once medical and menstrual history is reviewed, the next step is to undergo various blood tests and diagnostic procedures to determine overall health status and - most importantly - hormonal levels.
Blood tests can be helpful in pinpointing the underlying cause of ovulation issues. They might include a complete blood count (CBC) and complete metabolic profile, which checks for levels of blood cells, electrolytes, liver function, etc. They can also test a wide range of hormones, such as those related to reproductive and thyroid function, among others.
Transvaginal ultrasound can be used to examine the ovaries for structural abnormalities behind ovulation problems. It can also evaluate the presence or development stage of ovarian follicles that are released during the cycle.
Ovulation Problems Treatment

Ovulation can be induced in several ways, depending on the severity of the problem and the underlying cause. The most common approaches to ovulation induction include: lifestyle habits, alternative medicine, and conventional medicine.
Lifestyle Habits
Safely losing or gaining weight to reach an optimal BMI can promote hormonal balance as well as restart or regulate ovulation. It can be achieved through the following approaches:
Wholesome diet. Opting for foods rich in phytoestrogens, such as tomatoes, nuts, or beans, and full-fat dairy can fill in the nutritional gaps and support the endocrine system in overcoming hormonal issues.
Regular exercise. Avoiding strenuous exercises and focusing on moderate-level sports, such as jogging and swimming, can lead to healthy menstruation and regular ovulation.
Relaxation. Finding ways to reduce negative effects of high stress on egg release is essential to fixing abnormal ovulation. Good stress-relief methods include mediation or yoga.
Alternative Medicine
Phytoestrogenic supplements, like red clover, black cohosh, or ginseng, supply the body with plant-based estrogens to promote hormonal balance, regulating menstrual cycles and resolving ovulation issues.
Hormone-regulating supplements, like Macafem, nourish the endocrine system to optimize its hormone production, thus regulating monthly egg release and bringing an end to abnormal ovulation.
Medications & Surgery
- Fertility pills and injections, such as clomiphene citrate or metformin, act directly on hormone-producing glands to improve their function, resulting in regular ovulatory cycles.
Fertility surgery, including ovarian drilling and ovarian wedge resection, can resume regular ovulatory cycles, especially among women with PCOS.
Conclusions
There is no doubt that being diagnosed with ovulation issues can be the cause of significant stress and worry. This is especially true for those who have certain conditions before getting pregnant, such as diabetes, endometriosis, or PCOS, that might negatively affect their fertility. Fortunately, women with abnormal ovulation have a wide array of approaches to consider, from lifestyle changes and alternative medicine to infertility treatments that include assisted reproduction technologies (ARTs), like artificial insemination or IVF.
Sources
- Better Health Channel. (n.d.). Infertility in woman. Retrieved October 4, 2018 from https://www.betterhealth.vic.gov.au/health/ConditionsAndTreatments/infertility-in-women
- British Medical Journal. (2003). Anovulation. Retrieved September 28, 2018 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC192851/
- British Medical Journal (2007). Managing anovulatory infertility and polycystic ovary syndrome. Retrieved September 28, 2018 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1995495/
- National Collaborating Centre for Women's and Children's Health. (2013). Ovulation disorders. Retrieved September 28, 2018 from https://www.ncbi.nlm.nih.gov/books/NBK327781/
- Office on Women's Health. (n.d.). Infertility. Retrieved September 28, 2018 from https://www.womenshealth.gov/a-z-topics/infertility
- The Journal of Clinical Endocrinology and Metabolism. (2010). Oligoovulatory and Anovulatory Cycles in Women with Polycystic Ovary Syndrome (PCOS): What's the Difference? Retrieved October 5, 2018 from https://academic.oup.com/jcem/article/95/12/E485/2835423
- University of Toledo. (2009). What is the best first-line treatment for infertility due to anovulation in women with polycystic ovarian syndrome? Retrieved October 4, 2018 from https://utdr.utoledo.edu/cgi/viewcontent.cgi?referer=https://www.google.com/&httpsredir=1&article=1400&context=graduate-projects