About
What are Headaches?
Quick Facts about Headaches
- Over 99% of people will experience a troublesome headache at some point of their lives.
- Female prevalence of headaches dramatically increases between puberty and menopause.
- Before puberty, headaches are slightly more common in boys than girls
A headache, medically termed cephalalgia, is any pain or discomfort in the head. It can be localized to one area or felt around the head. It may also radiate to the neck.
There are several types of headaches, many of them recurrent, and each one produces a specific type of pain, many times involving a different part of the head.
It is estimated that women are three times more likely than men to suffer from chronic headaches, and this difference makes itself more noticeable during times of hormonal imbalance. Certain headaches are typical of PMS or become more prevalent during certain transitional stages of reproductive life, like puberty, pregnancy, post-partum (including breastfeeding), and menopause.
Identifying Headaches
When a headache occurs for no apparent reason, it is called a primary headache. When it presents itself as a symptom of another illness then it's called secondary headache.
Almost 90% of headaches are primary headaches, which can be very intense but are almost never dangerous. Primary headaches can vary in intensity, frequency, and the part of the head they affect, and they are very likely to be recurrent. They include tension-induced headaches and migraines, among others.
In order to understand the processes behind recurrent primary headaches, continue on to the next section to read about their hormonal and non-hormonal causes.

Causes
Learning about the causes of headaches provides the key to understanding how to prevent and treat these troublesome attacks. Although the exact causes of headaches -especially migraines- are complex and largely unknown, most doctors and researchers believe hormonal changes are the primary cause of migraines because of its increased prevalence among women. In addition to these completely normal hormonal causes, other factors and medical conditions can, in more rare instances, cause headaches.
Continue reading to learn more about the hormonal and additional causes of migraines and tension headaches.
Hormonal Causes of Headaches
Hormones are chemical messengers that control every process in the body, so when changes in these hormone levels occur, certain health disorders can arise. Medical researchers have found a link between fluctuating levels of hormones, especially estrogen, and an additional susceptibility to recurrent headaches.
The hormones estrogen and progesterone influence different functions all over a woman's body, from mood, to appetite, sexual desire, sleep and memory, and many of their ramifications are hidden or are still misunderstood. Women of reproductive age (from puberty to menopause) are three times more likely to suffer from migraines and tension-induced headaches. However, before puberty it is boys who are slightly more likely to suffer from headaches, and once they reach their post-menopausal years their incidence also decreases dramatically.
Furthermore, several large studies have pointed out headaches are much more prevalent the days before menstruation, and that even 3.9% of women experience them exclusively during those days. Headaches also increase significantly during pregnancy and during the period right before menopause. This is the reason why, while nobody knows exactly what sets off headaches, scientists believe female reproductive hormones play a large role in their appearance.
Furthermore, there are also specific hormonal causes and typical environmental factors which can explain the occurrence of headaches according to the stage of a woman's reproductive life in which this disorder appears, such as around PMS and during puberty, pregnancy, post-partum and menopause.
Hormonal Changes throughout a Woman's Life
PMS is a consequence of hormonal fluctuations linked to the menstrual cycle.
In addition to the cyclical symptoms experienced during PMS, women experience specific transitional periods that are strongly linked to an exacerbation or recurrence of headaches, especially migraines and tension-induced headaches.
Puberty is the stage in which a girl's body begins to produce reproductive hormones; these and other factors, such as school pressures and changes in body chemistry, contribute to headaches during puberty.
Pregnancy leads to extreme changes in the production of reproductive hormones, which along with other factors, like fatigue or exposure to triggers, can lead to headaches.
Postpartum and breastfeeding is another stage where reproductive hormones are imbalanced, leading to symptoms like headaches. Also, other factors can contribute to headaches in postpartum, like the return of menstrual periods.
Menopause is the stage in a woman's life when production of reproductive hormones naturally declines, signaling the end of a woman's fertility. As well as hormonal causes, other factors add to the reasons for headaches during menopause, including the experience of other symptoms of menopause.
Other Less Common Causes of Headaches
While hormonal imbalance is a major underlying cause of primary headaches during a woman's reproductive life, experts also point out that they can be caused by other, less common, underlying conditions, including type 2 diabetes and certain infections.
Keep reading to learn what these risk factors and triggers are that have such a profound effect on a woman's experience of headaches.

Risk Factors and Triggers
Risk Factors for Headaches
Some women are more likely than others to suffer from recurrent migraines or tension-induced headaches, for inherent psychological, behavioral and health reasons - such as obesity, stress, or consumption of certain substances. There are certain predisposing factors that can affect a woman's hormone levels and increase the chances that a woman will develop recurrent headaches during her reproductive life.
Triggers of Headaches
In addition to long term risk factors, migraines and tension-induced headaches can also be triggered by certain environmental phenomena and behavioral habits. Avoiding these environments or habits as much as possible may help to avoid the onset of migraine and headache attacks. These include habits like smoking and drinking alcohol, as well as other external triggers.
Continue reading to discover the symptoms and signs of headaches to be able to choose a treatment specific to its cause.

Signs and Symptoms
Different types of headaches often affect specific parts of the head, and they tend to be characterized by different sensations as well. However, many symptoms of headaches are common among women going through a phase of hormonal imbalance.
Common Symptoms of Headaches
- Pain affects just the top, just the front, or the sides of the head.
- Pain is either always present to a mild degree, or it comes and goes.
- Throbbing, dull pressure, or constant band-like pain around the head.
- Sometimes it is accompanied by trouble sleeping, mild muscle pain, or light and sound sensitivity
What other symptoms might occur with headaches?
Unlike regular recurrent headaches, migraines are easily misunderstood and confusing to diagnose, because they often appear as a cluster of symptoms surrounding a headache, instead of a headache alone. The symptoms are usually defined into phases or stages, known as Prodrome, Aura, and Postdrome phases.
Signs of Headaches
As opposed to the previously mentioned symptoms, that are easily noticeable by the patient herself, medical signs are measurable criteria that are usually assessed by a physician. The following medical signs of hormonal imbalance will most likely be taken into account by a physician when diagnosing headaches:
- Rapid or irregular heartbeat
- Fluctuating blood pressure
- Abnormal bone density reading
- Slightly elevated or reduced body temperature (not enough to constitute fever or hypothermia)
- Abnormal serum levels of estrogen, testosterone, luteinizing hormone, or follicle stimulating hormone
Diagnosis of Headaches
To diagnose and identify the cause of these headaches, a doctor must usually perform two procedures: a review of the patient's medical history and then a physical exam. In some cases, if necessary, the doctor also may order some tests, mainly to rule out more serious conditions.
Complications of Headaches
Although primary headaches don't present any life threatening complications, in certain cases the extreme pain experienced can still be debilitating and interfere with a woman's daily life. Many women find themselves forced to call in sick at work, skip social outings or fall short on family obligations.
Furthermore, frequent headaches may also decrease a couple's level of intimacy, and create social withdrawal and feelings of isolation.
Women who experience severe and frequent migraines or tension-induced headaches may wish to treat or even prevent them. Keep reading below to learn about how to prevent and manage headaches.

Prevention and Management
Preventing Headaches
While there is no single way to completely prevent migraine headaches, just as there's no way to stave off hormonal process relating to women's reproductive life, there are a few step that a woman can take to lessen her chances of developing severe headaches, or to minimize the impact or length of time that symptoms occur.
In this sense, lifestyle changes for prevention are extremely important, especially with regard to diet, exercise and healthy habits. Moreover, a woman may seek ways to complement these lifestyle approaches with the use of supplements that help to enhance the endocrine system and, therefore, help to prevent or ease the intensity of migraine attacks and other symptoms of hormonal imbalance. Continue reading to learn more about lifestyle changes for the prevention of headaches.
For women who are already going through the disorder, prevention may not be possible if headaches have already appeared. Fortunately, there are many ways to manage them in order to prevent the onset of new episodes, or to lessen the intensity of the symptoms. Keep reading to learn about the different ways to manage recurrent headaches.
Managing Headaches
Wherever a woman happens to be when experiencing a migraine or tension-headache attack, or when feeling the first symptoms of a Prodrome or aura phase, there are effective ways to instantly manage the problem. Making minor daily changes and avoiding triggers can make a huge difference for women who are trying to manage recurring headaches.
There are certain tips and tricks available that can help improve the experience of headaches, giving women the tools they need to cope with a sudden, intense headache. There are general tips that women of all ages can use, such as certain breathing techniques, spending more time with friends, or keeping a journal.
Alternative Management Tips for Headaches
Alternative treatments are also a great way to manage headaches. These treatments will not tackle the hormonal cause behind most women's recurrent headaches, but they are effective in reducing stress in the short and medium term. Alternative treatments for recurrent headaches include acupuncture.
While these measures often help reduce the frequency and intensity of migraine headaches, they are unable to treat the root of the problem, which is hormonal imbalance. However, there are several natural treatments that can treat the hormonal causes of migraine headaches. Please continue to the next section to learn more about treating headaches.

Treatments
For women who are going through a phase of hormonal imbalance, headaches are something to be expected, although in some cases the symptoms can become severe enough to interfere with daily life. Luckily, it is more than possible to find an effective treatment for headaches.
Three Approaches to Treat Headaches
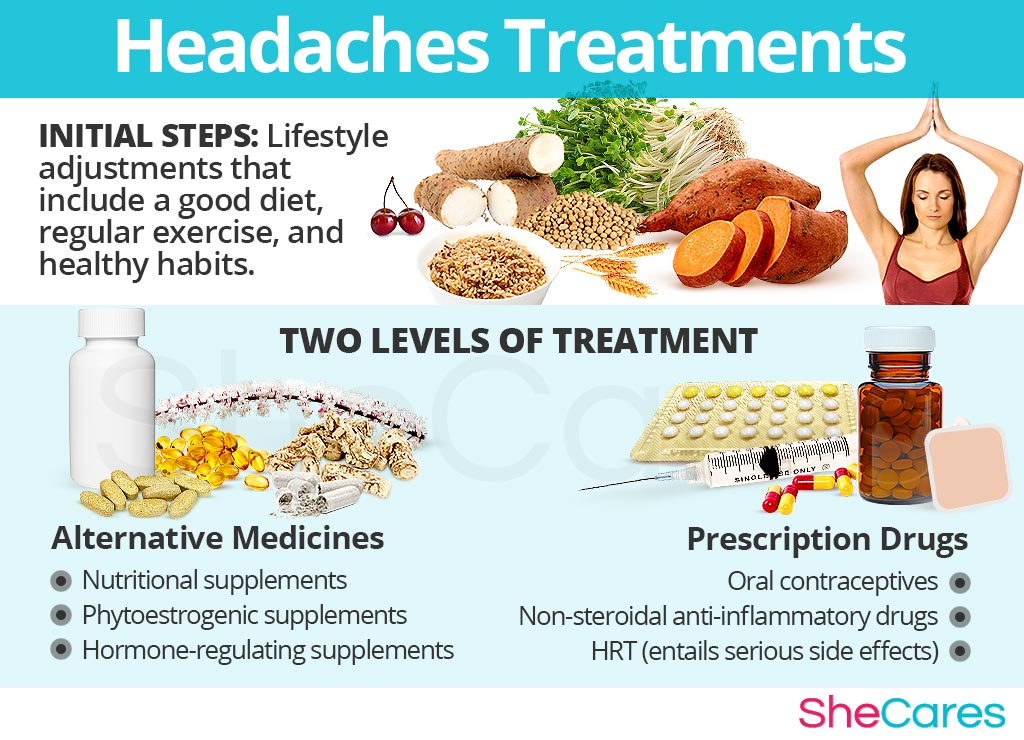
Three levels of approaches can be considered for treating headaches. These are categorized as: (1) Lifestyle Changes (2) Alternative Medicine, and (3) Pharmaceutical Options.
Women are encouraged to begin with the least risky approach to headaches treatment, lifestyle adjustments, and then proceed to alternative medicine. While medical intervention is not usually necessary to treat headaches, women who are unable to find relief from natural treatments may wish to consider pharmaceutical options, after properly assessing the risks associated with such a treatment.
Lifestyle Changes for Headaches
This primary level of treatment involves the least amount of risk, though conversely it requires the highest amount of self discipline. Often simple changes in lifestyle can reap huge benefits in fighting headaches, and achieving a higher overall level of health. Fundamentally, an improved diet, regular exercise, and healthy habits can do a woman great service.
While these changes will help alleviate headaches, they do not directly address hormonal imbalance - the most common cause of recurrent primary headaches - so further treatment may be necessary. Alternative medicine has proven to be an excellent way of treating headaches related to hormonal imbalance, like migraine and tension-induced headaches, in a safe and natural way.
Alternative Medicine
Alternative medicines and supplements involve little to no risk and can be an extremely effective way to treat headaches. In the case of herbal supplements, there are two main types that can be used: phytoestrogenic and hormone-regulating herbal supplements.
Phytoestrogenic herbal supplements
These supplements, such as black cohosh or dong quai, contain estrogenic components produced by plants that complement the low estrogen hormones in a woman's body, helping alleviate the fluctuations behind headaches. By introducing plant-based estrogens into the body, these herbs treat the underlying hormonal imbalance behind recurrent headaches like migraine.
They are mainly effective for menopausal women who are more likely to have low estrogen levels but are not necessarily effective for women in other stages of life such as puberty.
Hormone-regulating herbal supplements
These supplements, including Macafem stimulate the body's natural hormone production by nourishing the pituitary and endocrine glands, helping the whole hormonal system produce hormones more efficiently. This ultimately results in balancing not only estrogen but other important hormones such as progesterone.
These supplements can be considered the safest and most natural way to treat the underlying hormonal imbalance behind migraines and tension-induced headaches, and can be taken throughout a woman's life, as they support the body's natural hormone production.
Additionally, there are some other types of supplements that can also alleviate recurrent headaches, or at least make them more manageable, including dietary and other herbal supplements.
A combination of approaches is usually the most effective route to take. Lifestyle changes combined with alternative medicine will most likely be the best way to alleviate the symptoms of recurrent headaches and migraines. However, for some women the symptoms will be so severe that a more drastic treatment is necessary.
Pharmaceutical Options for Headaches
Interventions at the third level involve the highest risk and often the highest costs. Not all treatments are suitable for women at every life stage, so it is strongly recommended to speak to a licensed healthcare practitioner before starting any pharmaceutical treatment for recurrent primary headaches, or to rule out a more dangerous secondary headache.
There are three main types of pharmaceutical options that can be prescribed to treat recurrent primary headaches: hormone-regulating medication, pain-relieving medication and anti-seizure medication.
These three approaches are not mutually exclusive. A woman may use different approaches at different times or any combination of them, depending on the duration and severity of symptoms. Today more and more women find that dealing with symptoms of hormonal imbalance is best accomplished via a combination of healthy lifestyle and alternative treatments.
Sources
- Karli N., Baykan B., Ertas M., Zariföglu M., Siva A., Saip S. et al. (2012). Impact of sex hormonal changes on tension-type headache and migraine: a cross-sectional population-based survey in 2,600 women. Journal of Headache Pain, 13(7): 557-565.
- Lay C., Broner S. (2009). Migraine in women. Neurologic Clinics 27 (2): 503-11
- Mayo Clinic. (n.d.) Chronic Daily Headaches. Retrieved January 21, 2013 from http://www.mayoclinic.com/health/chronic-daily-headaches/DS00646
- Mc Gregor, A. (2007). Migraine in Pregnancy and Lactation: A clinical Review. Journal of Family Planning and Reproductive Care, 2007 : 33(2)
- Scheve T. (n.d.). 10 types of headaches. Retrieved January 21, 2013 from http://health.howstuffworks.com/diseases-conditions/headache/10-types-of-headaches.htm
- UK National Health Service. (2011). Hormone Headaches. Retrieved January 21, 2013 from http://www.nhs.uk/Livewell/headaches/Pages/Hormonalheadaches.aspx
- Vuković-Cvetković V., Plavec D., Lovrencić-Huzjan A., Galinović I., Serić V., Demarin V. (2010). Is iron deficiency anemia related to menstrual migraine? Post hoc analysis of an observational study evaluating clinical characteristics of patients with menstrual migraine. Croatian Clinical Acts, 49(4):389-94
- Wang S., Fuh J., Lu S., Juang K., Wang P. (2003). Migraine prevalence during menopausal transition. Headache, 43(5):470-8.




