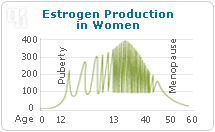
After the Women's Health Initiative (WHI) released a report in 2002 about the effects of postmenopausal estrogen, use of estrogen has changed. Further reports from the US Food and Drug Administration and the US Preventative Services Task Force had also issued recent recommendations against the use of estrogen for the prevention of chronic conditions. Below is a quick study of a woman who experienced hot flashes and is considering estrogen usage.
A healthy 49 year old woman with no previous poor medical history has been experiencing irregular menstrual periods for 6 months and an increase in hot flashes that interrupt her sleep pattern weekly. She is looking for a treatment method to ease her symptoms.
In considering estrogen, there are a few things she needs to know. She can either stick it out, as 30 - 50% of women experience an improvement in hot flashes after several months or she can take a risk and begin estrogen treatment as some women's hot flashes do not resolve within the predicted 4 -5 year mark.
Based on the 2002 research done by WHI this woman may already know the pros and cons that come along with estrogen usage:
Pros: Postmenopausal estrogen may prevent osteoporosis. Randomized controlled trials of estrogen reported an improvement in bone density among estrogen users. A reduction of fractures among estrogen users was displayed in women between 50 - 54 years of age. It should be noted however that use of non-estrogen prescriptions to treat osteoporosis is recommended over estrogen treatment.
Cons: Estrogen use may cause vaginal bleeding, breast tenderness, nausea, headaches, weight change, and a variety of other symptoms. It also increases the risk of coronary artery disease and stroke.
She can also consider alternatives to estrogen which include soy and red clover which are known remedies used to treat hot flashes though no substantial evidence can prove their efficacy. Black cohosh, dong quai, evening primrose oil, Chinese herbs and vitamin E are also used to treat hot flashes, but again effectiveness is subjective. Still, out of these alternatives, estrogen seems to be the most effective treatment for hot flashes.
If this woman decides to take estrogen her doctor will probably tell her that there is a range of doses available, subject to adjustment according to the presence of the problem and progress made. Her doctor should also tell her that after 2 - 3 years, estrogen dosage should decrease and eventually be discontinued.
Estrogen may be the most effective way to ease the hot flashes that come along with menopause. Estrogen however, is not without a slew of harmful and uncomfortable side effects. There are more natural alternatives to estrogen treatment for hot flashes, though estrogen seems to be the most effective. It is important for women considering estrogen treatment for hot flashes to consider the pros and cons of estrogen use and to sit down with their doctors to determine the right dosage. It is important to get off the treatment as soon as possible, and the lowest recommended dosage should always be prescribed.