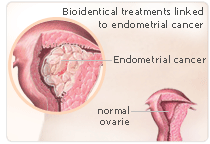
Bioidentical hormones have been touted as the safe, gentle, and effective alternative to traditional hormone replacement therapy (HRT), and have become especially popular since HRT has been proven to increase risk for cancer, stroke, and other significant health problems. The medical community has long warned that there is insufficient evidence to merit these claims for safety and efficacy, however, and their caution has now been justified: new research published in the Medical Journal of Australia has linked use of bioidentical hormones with three cases of endometrial cancer.
About bioidentical hormones:
Bioidentical hormones are touted as safe, “all-natural” hormones that are not prescribed at a one-size-fits-all dosage, like conventional HRT, but are tailor-compounded to meet individual hormonal needs. Allegedly in order to provide hormones at the lowest levels required, compounders of bioidentical hormones gauge each patient's hormonal levels via salivary testing, and then tweak the compound based on the results of the test.
Risks of bioidentical hormones:
Medical professionals have long proclaimed themselves wary of this progressively popular alternative treatment, warning that salivary hormonal tests are by no means reliable signs of a woman's hormonal levels. The “appropriate” hormonal levels for a postmenopausal woman established, so such a test has limited value, anyway.
Furthermore, there is no evidence that hormones from so called “natural” sources or that have been “custom compounded” are with lesser risk than or even as potent as standard HRT. The fact that the FDA (the governmental Food and Drug Administration) does not watch over or control the production of biodidentical hormones is another major worry of doctors.
Now, solid information that justifies years' worth of caution has just been published: a study in the Medical Journal of Australia describes three distinct cases of postmenopausal women (54, 59, and 71 years of age, respectively) taking bioidentical hormones who were subsequently diagnosed with endometrial cancer.
Eden, Hacker, and Fortune, the authors of this report, suggested a multitude of potential risks linked to bioidentical hormones. First of all, the compounding of bioidentical hormones is not supervised by any governing body, and the administration routes (like tablets, lozenges, or creams administered to the skin) have not been studied for usefulness.
The authors state that the most important factor, however, may be the practice of compounding the bioidentical hormones based on the results of salivary hormonal tests, which are not faithful gauges of hormonal levels. Due to this, the compounders may fail to add sufficient amounts of progesterone to the compound, which is vital to protect against the cancer-stimulating effects of estrogen alone. Alternatively, the administration routes may ease for the absorption of only estrogen, while progesterone was less fully absorbed.
Given the worrisome implications of this study on top of previous concerns about the untested safety of bioidentical hormones, health organizations and medical professionals strongly discourage the use of biodientical hormones, and encourage current users to undergo regular screening for cancer or other health complications.