
A study has been conducted to determine how and if certain hormone levels effect the sleep pattern in middle-aged women. 630 women of perimenopausal and premenopausal status. Aged 43 - 53 years old and from a majority of ethnic groups have been studied. After results of the women's journals were compared to their hormone levels, conclusions reveal that high levels of certain hormone do indeed negatively affect aging women's sleep.
It is a relatively known fact that sleep disorders come with age. For women aged 35 to 49 years old, poor sleep quality is associated with “lower follicular-phase plasma estradiol levels.” In the Daily Hormone Study portion of the Study of Women's Health across the nation, women were tested to determine if hormones were a cause of sleep disorders during menopause.
For one year, the women involved in the study recorded in their daily “bedtime diary” whether or not they had difficulty sleeping during the prior night. The diary contained 18 questions regarding sleep quality, mood, and physical and vasomotor symptoms. Their morning urine samples were used to determine levels of luteinizing hormone, follicle-stimulating hormone, estradiol metabolites, and progesterone metabolite. The findings were matched with the results of the hormone assays from the morning urine collection from the night before.
The 434 perimenopausal women (those who experienced no menstrual irregularity in the past 12 months) were affected by PdG level. The 196 premenopausal women (those who reported menstrual irregularity) had specific problems with a FSH level.
SLEEP
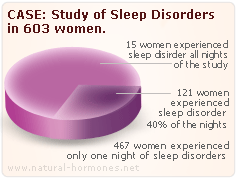
Of the 630 women, 467 reported difficulty sleeping on at least one night. 121 reported trouble sleeping on at least 40% of nights. On average, the women experienced trouble sleeping almost three nights a week, a statistic consistent with to insomnia and studies on sleep disorders. 15 women had trouble sleeping on all recorded nights. Sleep stability was influenced by menopausal status, particularly among women who experienced hot flashes.
The results for symptoms of sleep disorders were strongest at the beginning and end of the menstrual cycle. Mid cycle was the best sleep. 29% more of perimenopausal women had difficulty sleeping versus premenopausal women.
*Logistic regression was used with day of cycles as the time variable used to test/estimate the associations between sleep disorders and hormone levels.
*The criteria for the participants included 1) at least one ovary 2) an intact uterus 3) one menstrual period in the past months 4) no use of sex steroid hormones in the previous three months and lastly, 5) not pregnant.
The Study of Women's Health across the nation concluded in the Daily Hormone Study that hormones do affect the sleep patterns of mid-life women. Though the hormones differ in both premenopausal and perimenopausal women, each group was known to loose a considerable amount of sleep during the beginning and end of their menstrual cycles.