This article discusses numerous studies that have investigated the risks of hormone therapy which is commonly used to deal with problematic menopause symptoms caused by an imbalance of natural hormones. Although symptoms differ from female to female, many are uncomfortable and embarrassing. The loss of natural hormones like estrogen during menopause leads to a variety of unwanted symptoms. Hormone therapy (HT) is regarded as a highly effective treatment for correcting an imbalance of natural hormones and thus dealing with problematic menopausal symptoms. Yet, despite its success, HT has been linked to cardiovascular disease and breast cancer and this article looks at such risks in more detail.
After the publication of the heart and estrogen and progestin replacement study (HERS), which reported that HT increased the risk of coronary heart disease (CHD), many women stopped using HT to relieve early menopause symptoms and looked for alternatives to deal with the loss of natural hormones such as estrogen during menopause. Changes were also made to clinical guidelines to deter the use of HT among women with known or suspected CHD.
Despite the fact that there are many natural hormone products on the market, especially estrogen products, clinical guidelines do not help women in choosing one estrogen over another in order to treat early menopause symptoms. Hence, using data from related studies, some of which are detailed below, is necessary.
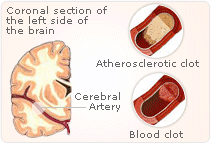
Although research carried out by Lemaitre et al suggests that the natural hormone EE is a little safer than CEE in terms of stroke risk, this research is not certain and does not change the fact that the WHI reported that the natural hormone estrogen (CEE), either alone or in combination with progesterone, increases the risk of stroke by around 40%. It can be assumed therefore, awaiting more evidence, that all estrogens are linked to increased stroke risks. Additionally, their effectiveness in easing early menopause symptoms can be considered equal.
It is important to carefully consider short-term HT use for replacing natural hormones and alleviating early menopause symptoms because the risk of stroke increases within the first 1 to 2 years of initiating HT. If indeed EE does carry lesser risks of cardiovascular disease than CEE, more women might be likely to choose EE to relieve early menopause symptoms. Though, this evidence is extremely weak and should not affect the decision of whether or not to use HT at all.
If considering using HT because other methods have failed to deal with early menopause symptoms, it is vital to understand both the benefits and risks of HT. Thought should also be given as to which natural hormone estrogen to use, as this may help reduce the risks of the treatment overall. A doctor is normally responsible for determining the estrogen used to treat early menopause symptoms, based on various medical criteria.
Choosing the most appropriate menopausal treatment to replace lost natural hormones depends on many things, including risks, preferences, and objectives. While data on the differences between natural hormones EE and CEE on cardiovascular disease risk is inconclusive, combined with other evidence, it suggests that EE may be slightly safer than CEE. If considering using HT to correct natural hormone imbalance during menopause, a consultation with a doctor is recommended. Furthermore, particular consideration should be given to the type of natural hormone estrogen to use in dealing with troublesome menopause symptoms, as this could reduce the risks of the treatment overall. Meeting with a medical professional will help educate women and allow them to make an informed decision about how best to treat the loss of natural hormones such as estrogen during menopause.