About
Quick Facts about Dark and Velvety Skin Patches
- This disorder typically occurs in women younger than 40.
- AN is not contagious, nor is it harmful to the skin itself.
- Dark underarms are usually a sign of an underlying hormonal disorder.
The emergence of dark and fuzzy areas on the skin is linked to excess levels of the hormone insulin in the bloodstream. This chemical messenger in the body is responsible for carrying glucose (sugar) from the blood into cells. Too much insulin is a sign of insulin resistance, a condition in which the cells are not sensitive and do not accept insulin. Consequently, the excess insulin stimulates certain cells to make the skin thick, velvety, and dark.
Insulin resistance is usually related to another disorder, such as polycystic ovary syndrome (PCOS) or obesity. Nonetheless, the significant hormonal shifts that occur during the different stages of reproductive life - puberty, pregnancy, post-partum (including breastfeeding), and menopause - can also have an effect on insulin levels. Ultimately, an increase in insulin can provoke unwanted dark skin patches.
In other instances, the appearance of a different skin condition known as melasma may occur in women. Melasma causes brown to gray-brown patches, usually appearing on the face, and is more common in darker-skinned women. In comparison to AN, melasma can also be caused by hormonal fluctuations, but the condition is generally triggered by exposure to excessive sunshine or irritation from new skin care products.
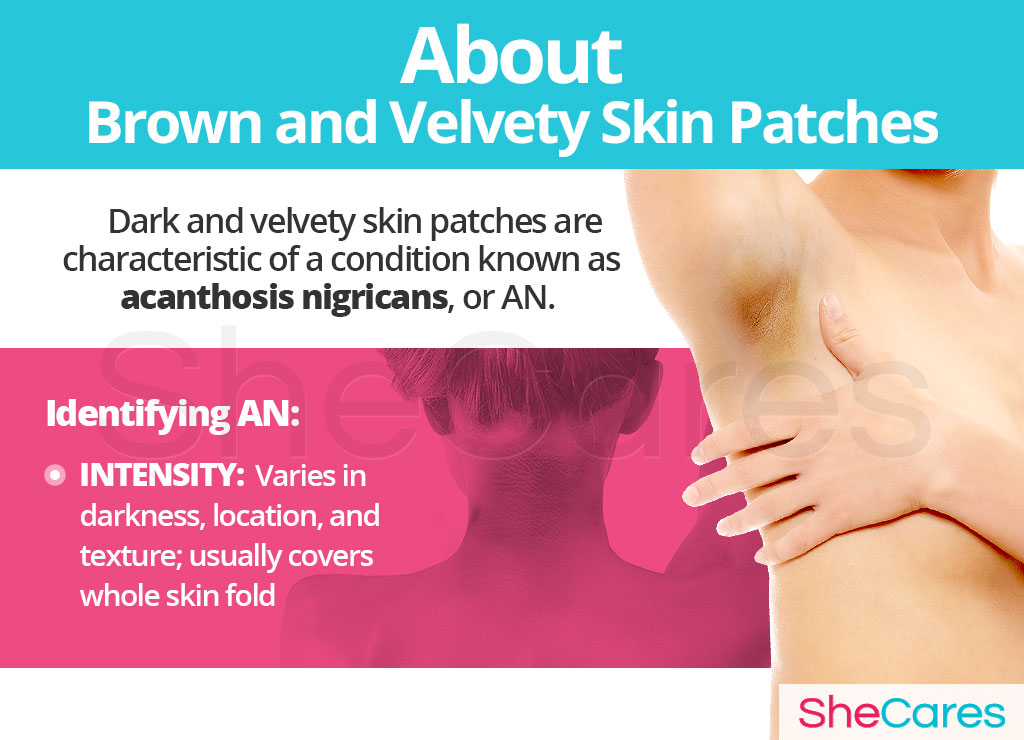
Identifying Brown and Velvety Skin Patches
Typically, AN appears as darker and thicker patches in the skin folds with a distinct texture. It may feel like velvet or peach fuzz. It most commonly occurs on the underarms, neck, and inner thighs. The exact appearance and location of the affected skin will vary from women to women. In many cases, grading the intensity of the disorder can help with its identification.
To better understand the various causes behind dark and fuzzy spots, continue reading the next section.
Causes
In order to be able to appropriately manage and treat dark skin patches, it is essential to understand the causes behind them. In the majority of cases, the primary cause is a hormonal imbalance, particularly of insulin in the bloodstream. In addition to excess insulin, there are some other causes of AN in less common cases.
Read further to learn more about both the hormonal and additional causes of soft and brown skin patches.
Hormonal Causes of Brown and Velvety Skin Patches
The dark skin patches are caused by a different hormone imbalance: an excess of insulin, the hormone that regulates the body's use of sugar. Insulin resistance - which is a hormonal disorder in and of itself - means that cells cannot take up the insulin produced in the body or the sugar that insulin carries to those cells. In response, the body produces more insulin in an attempt to deliver sugar, which is needed for energy, to the cells. The increased levels of insulin in the bloodstream can have negative effects, such as the dark patches of acanthosis nigricans.
The free-floating insulin may stimulate certain skin cells to replicate, or produce more of the same type of cell. This results in an excess of that material, causing skin abnormalities. For example, the extra insulin can trigger the production of the type of cell that makes the pigment melanin. These newly produced skin cells carry out their function to manufacture melanin, which results in the darkening of patches of skin. Likewise, insulin can stimulate the replication of the skin cells that produce keratin, a protein that makes up nails and hair and a key component of the outer skin layer. The excess of keratin produced by the new cells creates thickened skin and a fuzzy or velvety texture.
While brown velvety patches are linked more closely to changes in insulin level than fluctuations of sex hormones, the emergence of AN can be affected by the natural hormonal changes that happen during the reproductive stages of a woman's life: puberty, pregnancy, post-partum, and menopause.
Puberty, when a girl's body starts producing reproductive hormones, often brings the first hormonal changes and imbalances in a young woman's life. These natural fluctuations can also affect insulin levels.
Pregnancy involves great changes in hormone levels and with them great changes in the body. The fluctuation of hormones can have an effect on metabolism, which can lead to brown skin patches.
Post-partum and breastfeeding is another stage in which hormones are fluctuating constantly. This can lead to a continuation of the dark skin patches that appeared during pregnancy.
Menopause refers to the stage in a woman's life in which hormone levels naturally decline as the fertility period comes to a close. Dark and fuzzy patches can also appear during these stages.
Other Less Common Causes of Brown and Velvety Skin Patches
While most cases of fuzzy skin patches are related to an insulin imbalance, in some cases, a less common cause may be behind the emergence of AN.
Continue reading to learn about certain risk factors and external triggers that can make a woman more prone to having dark, soft skin patches.

Risk Factors and Triggers
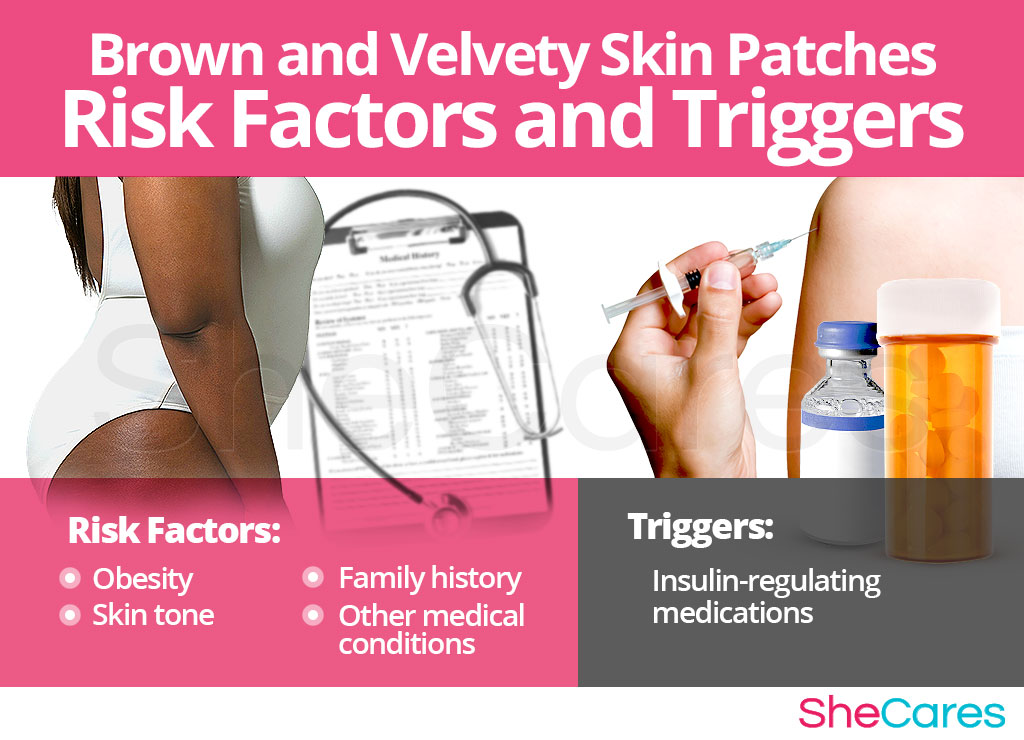
Risk Factors for Brown and Velvety Skin Patches
Some women are more likely to develop dark skin blemishes than others because of certain health and personal reasons, such as obesity and genetics. These risk factors can affect a woman's hormones and increase the likelihood of developing dark skin spots.
Triggers of Brown and Velvety Skin Patches
In addition to long term risk factors, dark skin patches can flare up suddenly because of certain triggers. Avoiding insulin-related medications as much as possible will reduce the incidence or recurrence of dark patches on the skin.
Keep reading to find out more about the signs and symptoms of brown skin patches and to choose a treatment specific to its cause.
Signs and Symptoms
Natural hormonal fluctuations will affect each individual woman differently throughout the course of her reproductive life. Dark, velvety spots may appear on different areas of the skin. However, there are some common symptoms that the majority of women have.
Common Symptoms of Acanthosis Nigricans
- Dark, velvety skin patches
- Patches on creases and folds, such as the armpits, neck, and groin
- Occasionally patches appear on the joints of the fingers and toes
The symptoms of this disorder only appear on the skin; there are no internal symptoms. Those with more severe cases may experience additional symptoms, including itchy or bad-smelling skin.
Signs of Brown and Velvety Skin Patches
Visible and palpable changes in skin coloration are the only sign of a hormonal imbalance that causes dark skin patches. Frequently, AN itself is sign of an internal hormonal disorder, such as polycystic ovarian syndrome or type II diabetes.
Diagnosis of Brown and Velvety Skin Patches
To diagnose and identify the symptoms of brown fuzzy skin, a doctor or dermatologist typically performs a simple skin exam. In some less common cases, they may also run some tests, especially if an underlying hormonal condition is the suspected cause.
Complications of Brown and Velvety Skin Patches
In rare cases, dark skin patches can be linked to dangerous internal complications. The presence of fuzzy dark skin patches usually points to an underlying internal condition. Though it is very rare, AN can be an indicator of cancer, especially stomach cancer.
Women who have large or embarrassing dark patches - especially on the underarms or neck - may wish to learn how to treat or prevent them. Continue reading to find some useful prevention methods and management techniques that may help with brown, fuzzy patches.

Prevention and Management
Preventing Brown and Velvety Skin Patches
There is no single, surefire way to fully prevent dark, velvety skin patches, because there is no way to hold back the body's natural hormonal processes. However, there are some steps a woman can take to reduce the chances of developing dark skin patches or to minimize their appearance.
An important means of prevention is lifestyle changes, especially concerning diet, exercise, and healthy habits. Additionally, lifestyle adjustments can be complemented with supplements that help enhance the functioning of the endocrine system and thus prevent or lessen hormonal imbalances.
In some cases, prevention may not be possible. If dark skin patches have already appeared, there are some management techniques that can help to reduce the intensity of the brown and fuzzy areas. Continue reading to learn more about ways that dark patches can be managed or lessened.
Managing Brown and Velvety Skin Patches
Some women may find dark patches embarrassing or be unable to wear sleeveless shirts, although the majority of women do experience the appearance of some spots during the hormonal changes throughout their lifetimes. They may wish to manage or mask velvety patches once they have emerged. Losing weight or applying makeup can help manage the appearance of brown fuzzy patches.
Read on to learn more about the various treatments for dark, velvety skin patches to find which may be most effective based on the underlying cause.

Treatments
Dark and fuzzy skin patches - which are most commonly causes by an imbalance of the hormone insulin - can be frustrating, embarrassing, and even itchy or smelly. Fortunately, there are many possible treatments for abnormal brown skin patches, geared to both the skin's surface and the underlying insulin resistance. The most effective treatment depends on the associated condition as well as the individual woman.
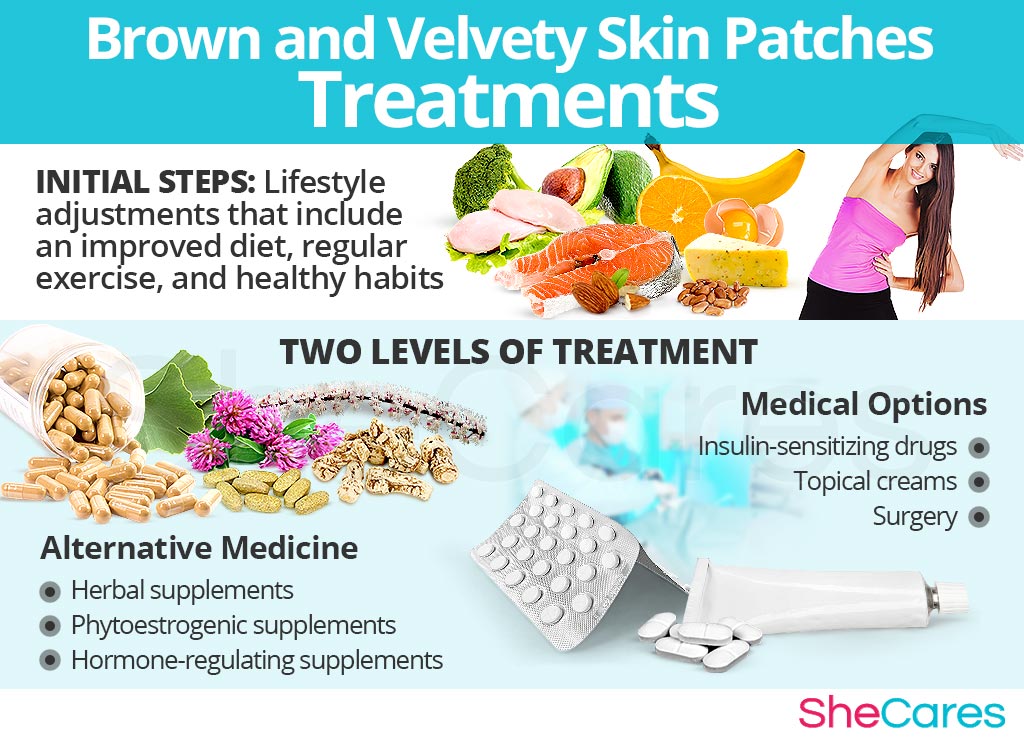
Three Approaches to Treat Brown and Velvety Skin Patches
Three levels can be considered for treating dark fuzzy skin patches. These are categorized as: (1) Lifestyle Changes, (2) Alternative Medicine, and (3) Pharmaceutical and Surgical Options.
Women are urged to begin with the least risky approach to treating velvety skin patches - lifestyle changes - before they try the next level of treatment. Pharmaceutical treatment is not always necessary to treat AN, but women may wish to receive medical advice about the associated condition. Women who are unable to find relief though alternative medicine and lifestyle adjustments may want to consider pharmaceutical options, but only after fully assessing the risks that come with such treatments.
Lifestyle Changes for Brown and Velvety Skin Patches
The first level of treatment involves the least amount of risk, but it entails the highest amount of self-discipline. In many cases, simple lifestyle changes can lead to healthier metabolism and the fading of dark patches. Generally, a good diet and exercise can help in treating insulin resistance and fuzzy skin patches.
Though these lifestyle changes may help reduce or eliminate the appearance of dark patches, they do not fully treat the hormonal imbalance that commonly lies behind the emergence of dark spots in all cases. Therefore, further treatment may be necessary. Alternative medicines have proven to be a tremendous way of treating velvety skin patches related to hormonal fluctuations in the body safely and naturally.
Alternative Medicine for Brown and Velvety Skin Patches
Alternative medicine and supplements involve little to no risk and can be a very effective means of treating dark skin patches. In terms of herbal supplements, there are two main kinds that can be utilized: phytoestrogenic and hormone-regulating supplements.
Phytoestrogenic herbal supplements
These supplements contain estrogens produced by plants, which function as a complement or replacement for estrogen in a woman's body. The introduction of these plant hormones treats the estrogen deficiency that could be the cause of dark blotches. An example of such a supplement is black cohosh.
These treatments are more effective for women going through menopause, since they are more likely to have low estrogen levels; therefore, these supplements are not necessarily as efficacious for women in other life stages, such as pregnancy, or those whose symptoms are based on insulin resistance.
Hormone-regulating herbal supplements
These supplements, including Macafem, stimulate natural hormone production by supporting the endocrine glands, which in turn helps the body produce hormones more efficiently and at the right levels. This results in a balance of hormones in the body, not just an addition of estrogen.
This type of supplement is considered the safest and most natural way of treating the basic hormonal imbalance that causes many dark spots. In addition, they can be used throughout a woman's life as they promote natural hormone production.
There are some other kinds of supplements that can also eliminate the appearance of dark patches or at least lighten them, including vitamins and other herbal supplements.
A combination of these two approaches - lifestyle changes along with alternative medicine - is likely to be the most effective way of reducing the appearance of dark and fuzzy skin patches. However, sometimes the symptoms will be so severe or persistent that a more drastic treatment becomes necessary.
Pharmaceutical and Surgical Options for Brown and Velvety Skin Patches
Treatment at the third level involves the highest risk and is often the costliest. Not all treatments are appropriate for women at a given life stage. So, it is highly recommended to consult a licensed medical professional before starting any pharmaceutical treatments for dark patches on the skin folds. In addition, some treatments may require a doctor's prescription.
Some pharmaceutical treatments may address the hormone imbalance while others only treat the outward symptoms. Some of the prescription medications may also be meant to treat some aspect of the underlying disorder. So, they may or may not target the hormonal imbalance. The various pharmaceutical and surgical options include insulin-sensitizing drugs, topical creams, and tumor removal, depending on the cause.
These three approaches to treatment - lifestyle changes, alternative medicine, and pharmaceutical options - are not mutually exclusive. A woman may choose to employ different approaches at different times or a combination thereof, depending on the severity of the symptoms. However, many women find that their symptoms are best alleviated through a combination of healthy lifestyle and alternative medicine treatments.
Sources
- American Academy of Dermatology. (n.d.). Acanthosis nigricans | Melasma. Retrieved November 3, 2017, from https://www.aad.org/public/diseases/color-problems/acanthosis-nigricans#overview | https://www.aad.org/public/diseases/color-problems/melasma#causes
- Braun, L. & Cohen, M. (2010). Herbs and Natural Supplements Inkling: An Evidence-Based Guide, 3rd Edition. Australia: Elsevier. Available from Google Books.
- Dahlgren, J. (2006). Pregnancy and insulin resistance. Metabolic Syndrome and Related Disorders, 4(2), 149-152. doi: 10.1089/met.2006.4.149
- Hermanns-Lê, T. et al. (2004). Acanthosis nigricans associated with insulin resistance: pathophysiology and management. American Journal of Clinical Dermatology, 5(3), 199-203. Retrieved November 6, 2017, from https://www.ncbi.nlm.nih.gov/pubmed/15186199
- Kobaissi, H.A. et al. (2004). Relation Between Acanthosis Nigricans and Insulin Sensitivity in Overweight Hispanic Children at Risk for Type 2 Diabetes. Diabetes Care, 27(6), 1412-1416. Retrieved November 6, 2017, from http://care.diabetesjournals.org/content/diacare/27/6/1412.full.pdf
- Mayo Clinic. (2015). Acanthosis nigricans. Retrieved November 3, 2017, from https://www.mayoclinic.org/diseases-conditions/acanthosis-nigricans/basics/definition/con-20025600
- National Organization for Rare Diseases. (n.d.). Acanthosis Nigricans. Retrieved November 6, 2017, from https://rarediseases.org/rare-diseases/acanthosis-nigricans/
- NHS. (2015). Acanthosis nigricans. Retrieved November 3, 2017, from https://www.nhs.uk/conditions/acanthosis-nigricans/
- Shane-McWhorter, L. (2009). Dietary Supplements for Diabetes: An Evaluation of Commonly Used Products. Diabetes Spectrum, 22(4), 206-213. doi: 10.2337/diaspect.22.4.206
- Sonagra, A.D. et al. (2014). Normal Pregnancy – A State of Insulin Resistance. Journal of Clinical & Diagnostic Research, 8(11), CC01-CC03. doi: 10.7860/JCDR/2014/10068.5081
