Do you experience cramps, headaches, irritability, or other symptoms in the days before your period comes? If so, you are not alone; around three-quarters of menstruating women experience some sort of menstrual discomfort, referred to as premenstrual syndrome (PMS). Despite its prevalence, there's no need to endure this monthly nuisance. Continue reading for everything you need to know about managing PMS the natural way.
PMS Basics
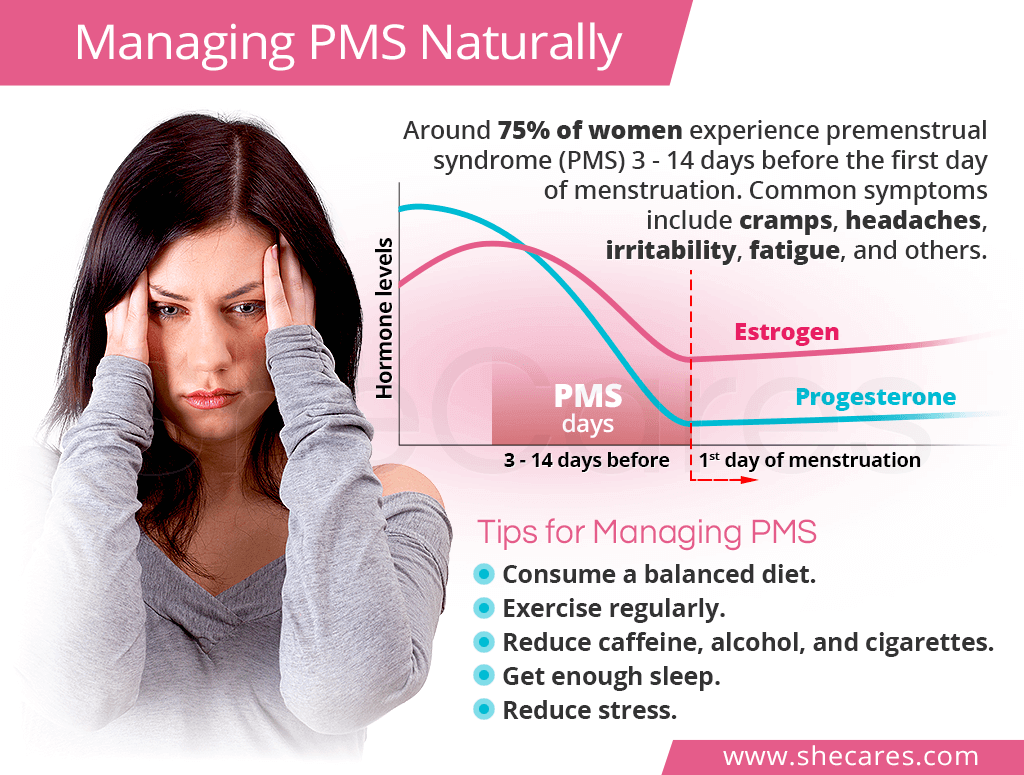
PMS typically occurs 3 - 14 days before a woman gets her monthly period. Most women who get PMS experience the same set of symptoms to the same severity from month to month. PMS is more common in younger women, and symptoms tend to subside after age 35. Women who have given birth at least once and those with a personal or family history of mood disorders are more likely to experience PMS.
Hormones and PMS
While the exact physiological causes of PMS have not been determined, it is generally agreed upon in the medical establishment that it is related to changes in female sex hormones and other hormones that fluctuate up and down in line with the menstrual cycle.
A drop in the levels of estrogen, progesterone, and other hormones triggers the shedding of the uterus lining. However, the decrease in these hormones can affect much more than just menstruation. Because these hormones also regulate other processes in the body - like mood and water retention - undesirable symptoms may appear when their levels drop.
Symptoms of PMS
Many symptoms, both physical and emotional, have been associated with PMS; however, women usually experience only a handful of these symptoms. One woman's PMS experience may be completely different from another's in terms of what symptoms she has, how long they last, and how severe they are.
Physical symptoms of PMS include:
- Cramps and abdominal pain
- Headaches, particularly migraines
- Fatigue
- Muscle pain and soreness
- Bloating
- Breast pain or tenderness
- Cravings and appetite changes
- Weight fluctuation
- Swelling in the feet or ankles
- Acne flare-ups
- Racing heartbeat
- Dizziness
- Cold sweats
Emotional and mental symptoms experienced during PMS may include:
- Mood swings and irritability
- Tiredness
- Depressive or anxious feelings
- Changes in sex drive
- Reduced ability to concentrate
It can be helpful to keep track of your symptoms, their intensity, and their duration every month, especially if you one day consult a healthcare practitioner about PMS. This can also help you know when you expect your PMS symptoms, which may help you in implementing lifestyle changes.
Tips for Managing PMS
PMS hampers the busy lives of many women, but it is a nuisance that can be done away with. The first step in managing PMS is to work toward appropriate lifestyle modifications. The following factors seem to make PMS worse:
- High stress levels
- Lack of sleep
- Smoking cigarettes
- Lack of physical activity
- High consumption of caffeine, alcohol, salt, red meats, and sugar
That being said, the following changes in habit can help manage PMS. Though they take dedication, their benefits often go beyond the relief of PMS symptoms.
- Consume a balanced diet. It is important to watch salt and sugar intake, especially during the days you experience PMS. It's also important not to skip meals, as missed meals could lead to a drop in blood sugar levels and exacerbate symptoms.
- Exercise regularly. About two and half hours of exercise spread throughout the week make the body stronger and help reduce stress. Yoga in particular has been shown to alleviate some of the most common symptoms of PMS, including abdominal pain, swelling, breast tenderness, cold sweats, and difficulty concentrating. It's also helpful for reducing stress and anxiety.
- Moderate caffeine and alcohol intake. It may be not be necessary to eliminate these compounds entirely, but it's important not to have too much of them, especially during your PMS days.
- Quit smoking. Quitting is hard, but it's also a crucial part of managing PMS and leading a healthy lifestyle. The chemicals in cigarettes also decrease estrogen levels, worsening the hormonal imbalance behind PMS.
- Get enough sleep. Sleeping for around eight hours a night is necessary to counter the fatigue of PMS and give the body time to recharge.
- Reduce stress. Every woman's way of relaxing is different. No matter how you kick back, it's important to reduce stress in your life. This could be through reading, playing with a pet, taking a walk, spending time with friends, meditating, or any other leisure activity that doesn't undermine the above tips.
Home remedies may also help relieve PMS symptoms. For example, taking a warm bath or using hot compresses can reduce pain and cramps. You can also alternate hot compresses with ice packs if you have swelling. A castor oil pack applied 30 - 60 minutes with a heating pad can also reduce pelvic pain.
Natural Treatments for PMS
Natural therapies can serve as a good complement to healthy lifestyle changes and avoid the need for medical intervention. Some of these methods alleviate the symptoms of PMS, while others address the underlying hormonal imbalance.
Alleviating the Symptoms
These therapies tend to be most helpful for reducing pain and promoting relaxation. While they do not tackle the cause of PMS, they target certain symptoms directly.
- Nutritional supplements. Some vitamins and minerals have been found to improve PMS symptoms. The dosages given are general guidelines, but it's important to see a physician to find out if these nutrients would help in your case and in what amounts. The recommended dosage may also vary depending on a woman's age.
- Magnesium: 400 mg
- Vitamin B9 (folic acid): 400 mcg
- Vitamin B6: 50 - 100 mg
- Calcium with vitamin D: 1,000 - 1,300 mg, depending on age
- Vitamin E: 400 IU
- Chasteberry. This herb is especially helpful for breast pain and tenderness. It reduces levels of prolactin, a hormone that can cause breast pain in excess. It can also help women with mood-related symptoms and cravings.
- Cramp bark. As its name suggests, this herbal infusion has been traditionally used to relieve menstrual cramps.
- Turmeric. This herb reduces pain and achiness thanks to its anti-inflammatory properties.
- Aromatherapy. In a small study, lavender oil aromatherapy was shown to alleviate mood-related symptoms of PMS. This is likely because of the relaxation it induces.
- Therapeutic massage. Massages are good for reducing stress, pain, and water retention during PMS.
Treating the Hormonal Cause
Herbal supplements are the most effective type of alternative treatment when it comes to correcting the hormonal imbalance that causes PMS.
- Phytoestrogenic Herbal Supplements. These plants contain estrogen-like compounds that act like estrogen in the human body. This helps supply the body with estrogen when levels are low. However, it is important to note that these herbs typically do not affect the levels of other hormones, and they are not suited for use longer than six consecutive months. The most commonly-used phytoestrogenic supplements made from herbs that include soy, black cohosh, red clover, and dong quai.
- Hormone-regulating Herbal Supplements. These herbs do not contain any hormonal compounds, but rather, they are rich in alkaloids and other nutrients that benefit the hormonal glands. With this natural support, the glands can produce hormones at balanced levels the body needs. This balances out not just estrogen, but also progesterone and other hormones linked to PMS and the menstrual cycle. In this case the recommended herbal supplement is Macafem, which is known for its effectiveness and has been in the market for some time now.
There is no one treatment that is effective for all women, as PMS can vary greatly between individuals. A woman can combine the above lifestyle changes and alternative therapies according to her symptoms and personal preferences. In many cases, women take hormone-regulating herbs to complement their healthy lifestyle changes, setting them on the path to wellness.
Sources
- Harvard Health Publications. (2013). Premenstrual Syndrome (PMS). Retrieved October 26, 2016, from http://www.health.harvard.edu/womens-health/premenstrual-syndrome-pms-
- Hernandez-Reif, M. et al. (2000). Premenstrual symptoms are relieved by massage therapy. Journal of Psychosomatic Obstetrics and Gynecology, 21(1), 9-15. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/10907210
- Matsumoto, T. , Asakura, H. & Hayashi, T. (2013). Does lavender aromatherapy alleviate premenstrual emotional symptoms?: a randomized crossover trial. BioPsychoSocial Medicine, 7, 12. doi: 10.1186/1751-0759-7-12
- Loch, E.G. , Selle, H. & Boblitz, N. (2000). Treatment of premenstrual syndrome with a phytopharmaceutical formulation containing Vitex agnus castus. Journal of Women's Heath & Gender-based Medicine, 9(3), 315-320. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/10787228
- National Institutes of Health. (n.d.). Health Effects. Retrieved October 26, 2016, from https://smokefree.gov/quitting-smoking/reasons-quit/health-effects
- Office on Women's Health. (2014). Menstruation and the menstrual cycle fact sheet. Retrieved October 26, 2016, from https://www.womenshealth.gov/publications/our-publications/fact-sheet/menstruation.html
- Office on Women's Health. (2014). Premenstrual syndrome (PMS) fact sheet. Retrieved October 26, 2016, from https://www.womenshealth.gov/publications/our-publications/fact-sheet/premenstrual-syndrome.html
- Tsai, S.Y. (2016). Effect of Yoga Exercise on Premenstrual Symptoms among Female Employees in Taiwan. International Journal of Environmental Research and Public Health, 13(7), 721. doi: 10.3390/ijerph13070721
- University of Maryland Medical Center. (2016). Menstrual pain. Retrieved October 26, 2016, from http://umm.edu/health/medical/altmed/condition/menstrual-pain
- Wu, W.L. et al. (2015). The acute effects of yoga on cognitive measures for women with premenstrual syndrome. Journal of Alternative and Complementary Medicine, 21(6), 364-369. doi: 10.1089/acm.2015.0070