About Melasma
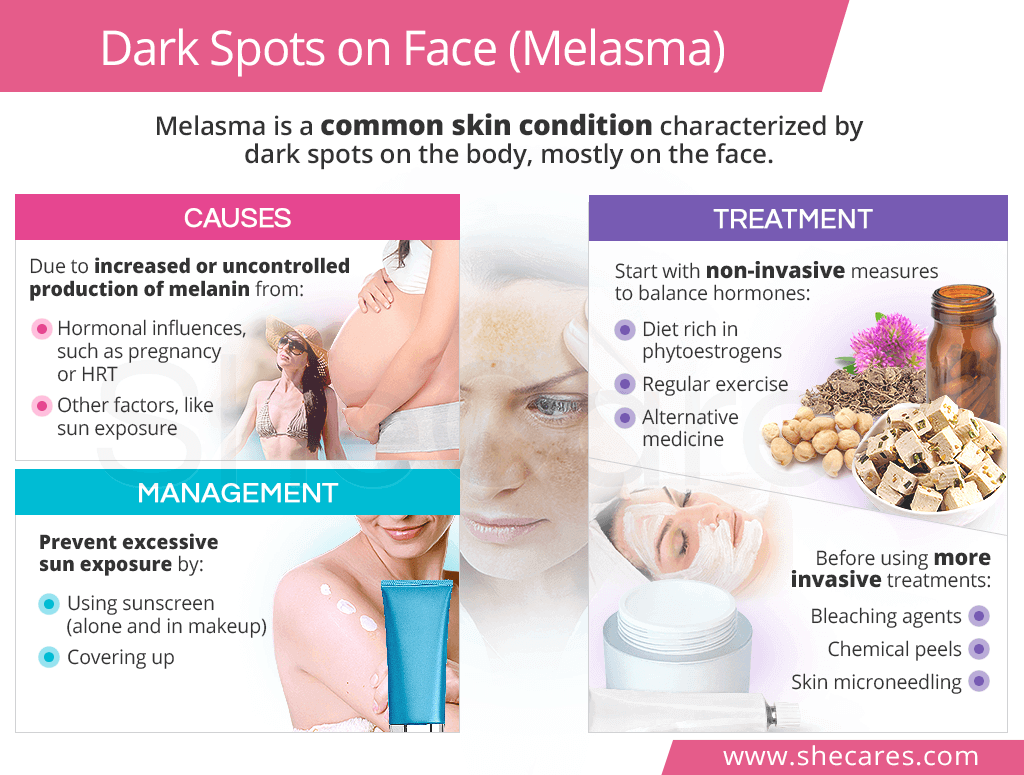
Melasma is a common skin condition that causes gray-brown patches to appear on the body, most commonly on the face, including on the chin, cheeks, upper lip, or bridge of the nose. It can also appear on other sun-exposed areas of the body, like the neck and forearms.
Furthermore, melasma has no other symptoms, meaning the condition is not associated with any itching, dryness, or other sensations. The only indication that a women has melasma is due to the condition's dark, patchy appearance.
That being said, while melasma is not life-threatening, many women wish to know exactly what they can do to manage and treat the dark spots on their face for aesthetic reasons. This starts with having a better understanding of their underlying causes.
Melasma Causes

Melasma occurs due to the increased or uncontrolled production of melanin, the most abundant skin pigment. While this often has hormonal influences, it can also be due to non-hormonal factors.
Hormonal Causes
An imbalance of reproductive hormones can trigger melanocytes (pigment-making cells in the skin) to produce additional melanin, giving rise to melasma.
This is why melasma is most common during pregnancy and is often referred to as chloasma, or the “mask of pregnancy.”2 Extreme fluctuations of estrogen and progesterone that ensue throughout the various stages of gestation to foster the health of the growing baby trigger the production of excessive melanin.
Additionally, exogenous hormonal treatments like oral contraceptives or hormone replacement therapy (HRT) can also trigger melasma in women.
Other Causes
The most common non-hormonal cause of melasma is sun exposure as ultraviolet (UV) sunlight stimulates melanocytes.
Because of the sun's role in the development of melasma, the skin condition is often worse in the summer in many women. Also, it can come and go year in and year out, even once hormones are under control.
Melasma Management
Many of the management techniques recommended for melasma deal with preventing excessive sun exposure. They include the following measures:

- Use sunscreen. Because sunlight can trigger melasma outbreaks, it is crucial that women wear sunscreen daily, even when it is cloudy. Opt for those with non-chemical blockers, like zinc or titanium dioxide, which prevent all light and wavelengths from penetrating the skin.
- Apply makeup with sunscreen. Some makeup brands include sunscreen in their formulas for UV protection. When paired with normal sunscreen, this will be an added bonus to further block out the sun's rays.
- Cover up. Remember that melasma isn't only confined to the face. Putting on a wide-brimmed hat will help shade your neck from harmful UV rays as well. Also, wear clothing that covers the shoulders and arms, too, especially if planning to spend quite a bit of time outdoors.
- Cleanse routinely. Because environmental pollutants can make skin more susceptible to sun damage and - thus - melasma, women should clean their skin nightly to remove particulate matter and offer it added protection.3
- Put on serum and moisturizer. Applying a serum with antioxidants, such as vitamins C and E, can hasten the healing process of the skin when damaged by the sun. Afterwards, apply a good moisturizer to restore the fat barrier of the skin.
While these methods will help bring temporary relief from melasma, long-term skin health will only be achieved once the underlying cause is treated.
Melasma Treatment
The best treatment for melasma often starts with non-invasive lifestyle changes - many of which are aforementioned - and then moves onto more risky pharmaceutical options if needed.
So, for women suffering from hormonal imbalance, enjoying clear skin starts by instilling non-invasive methods to promote endocrine system health, which can include:

- Optimizing the diet. Women should aim to consume a healthy balance of lean protein, healthy fats, and complex carbs, making sure their diet consists of plenty of fresh fruits and vegetables as well. Foods with phytoestrogens - plant-based estrogens - are often recommended for their hormone-balancing effects. Find them in soy products, chickpeas, flaxseeds, legumes, and more.
- Exercising regularly. Not only has exercise been praised throughout the years for its mood-boosting and bone-strengthening effects, but it is also beneficial for helping combat weight gain, fight depression and other mental health disorders, and improve sleep patterns. Strive for at least 30 minutes a day, five days a week, combining aerobic and strength-training routines.
- Using alternative medicine. Phytoestrogenic herbal supplements - like black cohosh and red clover - contain stronger concentrations of phytoestrogens to fight an estrogen imbalance that may be the culprit behind melasma. Yet, because they are not safe for long-term consumption, many women choose to turn to hormone-regulating supplements, like Macafem, which nourish the endocrine glands to stimulate natural hormone production.
If none of the aforementioned measures work, women may advance with medications and topical treatments to help lessen the appearance of melasma.
Some of the most commonly prescribed topical treatments include retinols and retinoid treatments, which hasten the body's natural cell turnover rate; bleaching agents like hydroquinone; or skin lightening agents like kojic acid or azelaic acid.
The most invasive treatments are chemical peels, laser treatments, or skin microneedling. Keep in mind that these last options may not work as well as claimed for getting rid of dark spots on the face.
Needless to say, it is of the utmost importance that women who are pregnant clear any treatment options with their overseeing medical practitioner before advancing.
Sources
- American Academy of Dermatology. (n.d.). Melasma: Overview | Signs and Symptoms | Diagnosis and Treatment | Tips for Managing. Retrieved August 20, 2019, from https://www.aad.org/public/diseases/color-problems/melasma
- American Pregnancy Association. (n.d.). Skin Changes during Pregnancy. Retrieved August 21, 2019, from https://americanpregnancy.org/pregnancy-health/skin-changes-during-pregnancy/
- Bagherani, N. et al. (2015). An Overview on Melasma. Pigmentary Disorders, 2(216). doi: 10.4172/2376-0427.1000216
- MedlinePlus. (2017). Benefits of Exercise. Retrieved September 9, 2019, from https://medlineplus.gov/benefitsofexercise.html
- Melnick, S. et al. (2016). Hyperpigmentation in a middle aged woman: a common yet underdiagnosed condition. Journal of Community Hospital Internal Medicine Perspectives, 6(3). doi: 10.3402/jchimp.v6.31544
- The Skin of Color Society. (2019). Melasma. Retrieved August 21, 2019, from http://skinofcolorsociety.org/dermatology-education/1406-2/
Footnotes:
- Famenini, S. et al. (2014). Finasteride Associated Melasma in a Caucasian Male. Journal of Drugs in Dermatology, 13(4), 484-486. Retrieved August 20, 2019, from https://jddonline.com/articles/dermatology/S1545961614P0484X/1/
- American Academy of Dermatology. (n.d.). Melasma: Who Gets and Causes. Retrieved September 9, 2019, from https://www.aad.org/public/diseases/color-problems/melasma#causes
- Harvard Health Publishing. (2018). Unmasking the causes and treatments of melasma. Retrieved September 9, 2019, from https://www.health.harvard.edu/womens-health/unmasking-the-causes-and-treatments-of-melasma