About IUD
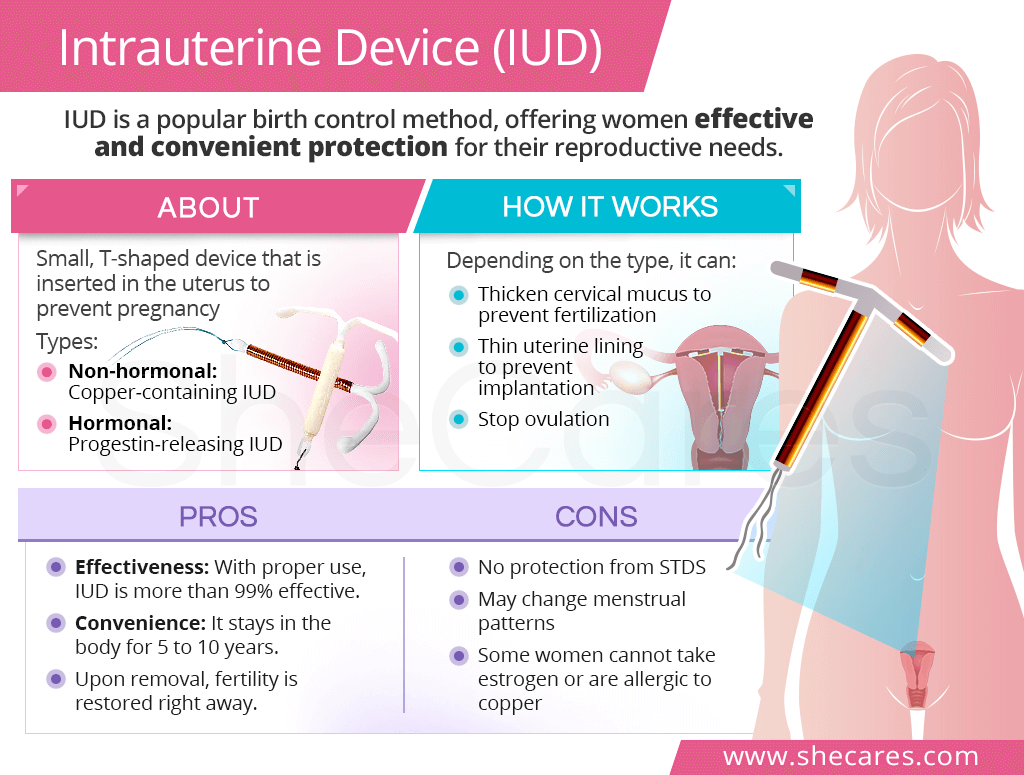
An intrauterine device, or IUD, is a small, T-shaped device that is inserted in the uterus to prevent pregnancy.
An IUD typically measures about 1 - 1.25 inches (29-32 mm) wide and 1 - 1.4 inches (3-36 mm) long.2 It also contains short strings made of thin plastic.
Types of IUDs
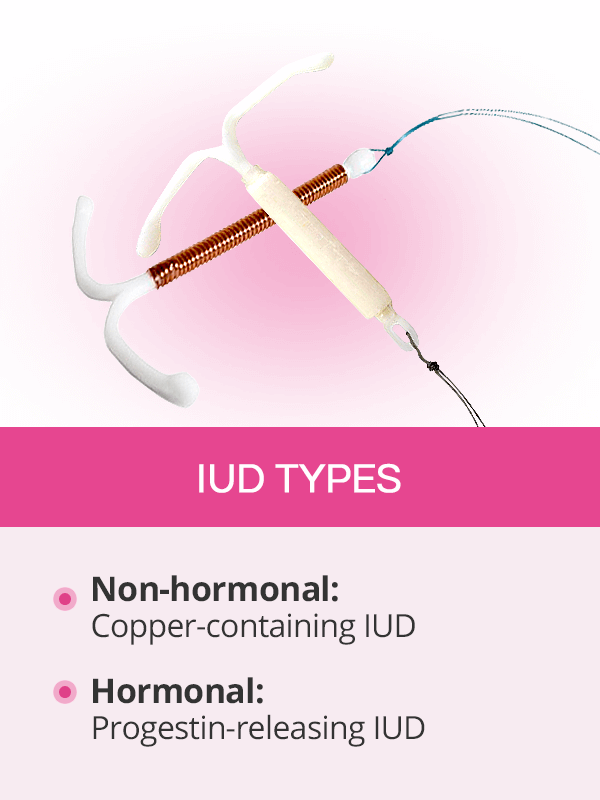
There are two types of IUDs women may consider for contraception, hormonal and non-hormonal.2
Hormonal IUDs. They are also called progestin-releasing IUDs and are available in three strengths: 12.5mg (approved for 3-year use) as well as 19.5mg and 52 mg (approved for 5-year use).
Non-hormonal IUDs. They are also known as copper-releasing IUDs (approved for up to 10 years).
IUD Insertion
IUD insertion is performed at a gynecologist's office at any point of the menstrual cycle. It takes a few minutes and generally does not require anesthesia, although it may be given locally. A pregnancy test and screening for sexually transmitted diseases (STDs) may precede the insertion.
The procedure itself consists of passing the IUD through the vagina and the cervix and placing it in the upper part of the uterus. Once positioned correctly, an IUD cannot be felt, except for a thin string that extends down the cervix and into the back of the vagina.
There are no major side effects following IUD insertion. Some women may experience mild cramping or spotting. A doctor will also typically schedule a follow up within four to six weeks to ensure that the IUD is correctly placed.
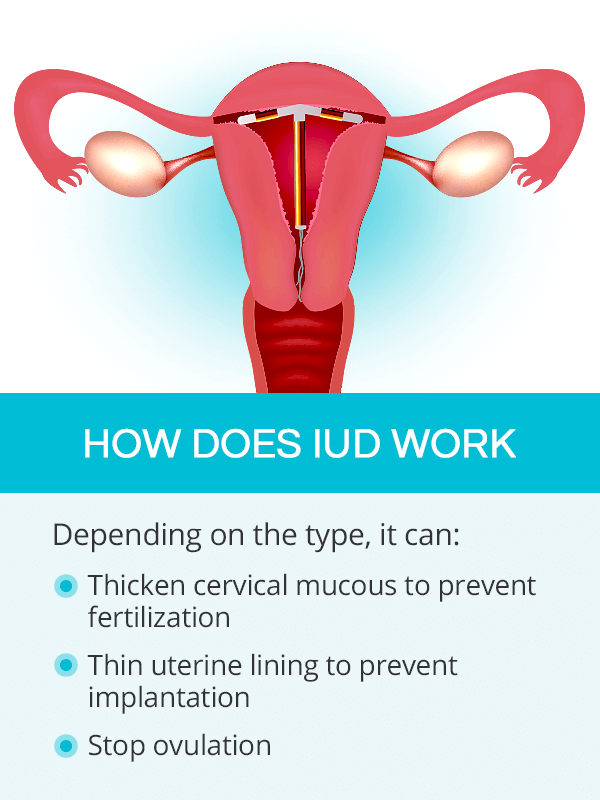
How Does an IUD Work
An IUD prevents pregnancy by releasing compounds that interfere with conception. The kind of compounds and the contraceptive mechanism will depend on IUD type:2,3
Characteristics:
Hormonal IUD
Non-Hormonal IUD
2) It stops ovulation
Since copper, or non-hormonal, IUD begins to work immediately after insertion, it can also be used as emergency contraception within five days after unprotected sex.4
IUD Pros and Cons

While an IUD is generally regarded as a convenient and reliable birth control method, there are significant limitations that might be unsuitable for women. The pros and cons of IUD include the following:
Pros of an IUD
- With proper use, an IUD is more than 99% effective.5
- It is long-lasting, providing protection for up to 10 years.
- Considering its long duration, IUD is cost-effective, especially if covered by health insurance.
- Upon removal, fertility is restored right away without delays.
- An IUD can be used when breastfeeding.
Cons of an IUD
- An IUD does not protect from STDs and is not recommended for those with untreated STDs.
- While it is a one-time cost every few years, an IUD insertion and other medical costs can exceed $1,300.5
- It may change menstrual patterns, like heavy periods with a copper IUD and light periods with a progestin IUD.
- Some women cannot take estrogen or may be allergic to copper.
- The IUD can be accidentally expulsed out of the body, especially in the first three months.2
- Rarely, an IUD can cause pelvic infection or perforation of the uterus.
- If a woman gets pregnant with an IUD, there is a higher risk of ectopic pregnancy.6
Key Takeaways
Studies have shown that IUD use has been significantly increasing in the last years, alongside birth control implants.7 There are two types of IUDs: a hormonal one that works for up to five years and a copper one that can provide contraception for up to 10 years. Following insertion, women can enjoy 99% effectiveness and convenience without major side effects. However, an IUD does not prevent STDs, may cause heavy or light periods, and may not be recommended for women with copper allergies or those who cannot take estrogen. Nevertheless, an IUD is considered a safe, convenient,long-lasting, and reliable option for many menstruating women.
Sources
- CDC. (2020). Birth Control Methods. Retrieved July 13, 2020 from https://www.cdc.gov/reproductivehealth/contraception/index.htm
- CDC. (2017). Intrauterine Contraception. Retrieved July 13, 2020 from https://www.cdc.gov/reproductivehealth/contraception/mmwr/spr/intrauterine.html
- Indian Journal of Medical Research. (2014). Intrauterine devices & infection: Review of the literature. Retrieved July 13, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4345753/
- Journal of Contraception. (2016). Intrauterine devices and risk of uterine perforation: current perspectives. Retrieved July 13, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5683155/
- Kids Health. (2018). The IUD. Retrieved July 13, 2020 from https://kidshealth.org/en/teens/contraception-iud.html
- Medline Plus. (2020). Intrauterine devices (IUD). Retrieved July 13, 2020 from https://medlineplus.gov/ency/article/007635.htm
Footnotes:
- International Journal of Women's Health. (2010). Long-term safety, efficacy, and patient acceptability of the intrauterine Copper T-380A contraceptive device. Retrieved July 13 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2971735/#:~:text=The%20intrauterine%20device%20(IUD)%2C,used%20reversible%20method%20of%20contraception.
- Stat Pears. (2020). Intrauterine device (IUD). Retrieved July 13 2020 from https://www.ncbi.nlm.nih.gov/books/NBK557403/
- Medline Plus. (2020). Deciding about an IUD. Retrieved July 13, 2020 from https://medlineplus.gov/ency/patientinstructions/000774.htm
- Office of Population Affairs. (2019). Intrauterine device (IUD). Retrieved July 13 2020 from https://www.hhs.gov/opa/pregnancy-prevention/birth-control-methods/iud/index.html
- Planned Parenthood. (n.d.). IUD. Retrieved July 13 2020 from https://www.plannedparenthood.org/learn/birth-control/iud/how-effective-are-iuds
- Contraception. (2018). Contraceptive method use in the United States: trends and characteristics between 2008, 2012 and 2014. Retrieved July 13, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5959010/
- FDA. (2020). Birth Control. Retrieved July 13, 2020 from https://www.fda.gov/consumers/free-publications-women/birth-control